According to the College of Podiatry, the average person walks 150,000 miles in their lifetime, so it’s important we look after our feet!
Horder Healthcare’s Mr Andrew Skyrme, an orthopaedic surgeon and specialist in lower limb problems, gives his advice on treating the most common foot conditions: bunions, arthritis of the big toe, plantar fasciitis, Morton’s Neuroma and flat feet in adults.
Bunions
What are bunions?
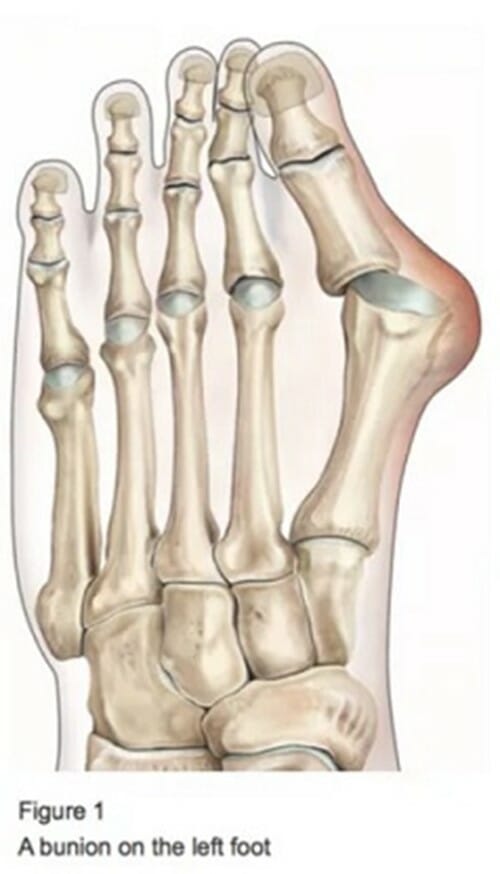
A bunion (hallux valgus), is a bony lump on the side of your foot at the base of your big toe. They’re not always painful but they can affect how you walk.
What causes bunions?
‘Your genes are definitely a factor in whether you’ll get bunions or not,’ says Mr Skyrme. ‘As are other factors such as wearing high heels which can cause changes in the front of your feet which cause weakness and make the bunion development worse.’ ‘They are also sometimes associated with arthritis of the joint at the base of your big toe.’
What can help people suffering from bunions?
• Self-help: ‘It’s not inevitable that you’ll need surgery – wearing wider fitting shoes can help,’ advises Mr Skyrme. Other self-help measures include using painkillers, bunion pads, orthotics and bunion splints which slip into the shoe – a podiatrist would be able to advise you on these.
• Surgery: In some cases though, you may need surgery to straighten your big toe so your foot can sit more comfortably in normal shoes. Most types of surgery take around six weeks to recover from. If you have bunions or think you may have, a podiatrist or orthopaedic consultant will be able to diagnose the condition and recommend treatment.
There are around 50 different surgical techniques for relieving bunions. The operation may involve removing the bunion, releasing or tightening ligaments around the toe, realigning your big toe, stiffening a joint and straightening your smaller toes. You can find out more in our bunion surgery page.
Arthritis of the big toe
What is arthritis of the big toe?
Most people know about arthritis in the major joints of the body like the knees, hips and shoulders. However, arthritis can affect any joint in the body, including your big toe.
Arthritis is usually caused by wear and tear of the joint. It tends to be painful and restrict movement of the big toe. Hallux Rigidus (which means stiff big toe in Latin) refers to difficulty in bending the toe upwards, and sometimes an extra bump of bone can form on the top of the toe, whilst Hallux Limitus refers to limited movement within the big toe.
What causes arthritis in the big toe joint?
Arthritis can affect anyone, but athletic types tend to be more prone to arthritis in the feet as the joint is more likely to come under stress. It causes pain in the big toe which feels worse when walking or running. Your doctor should be able to distinguish it from other causes of a painful big toe which may include gout, rheumatoid arthritis and diabetes.
What can help people suffering from arthritis of the big toe?
• Shoes: Try wearing insoles and protective silicone over the tender areas to protect the top of the big toe, as well as wearing shoes with a firm sole. Anti-inflammatory painkillers may also help.
• Manipulation and steroid injections: These can release stiffness in the joint allowing you to move it more and reduce pain. It reduces pain in about eight out of ten patients for up to 5 years.
• Cheilectomy: This is surgical removal of the “bump” on the top of the big toe, done under general anaesthetic as a day case procedure. Afterwards, you need to wear stiff-soled shoes for two weeks; pain and swelling may persist for several months though.
• Fusion: Bones in the big toe are surgically fused together and held in place with a plate or two screws. The body then grows new bone over the top. Recovery is usually about 6 weeks, although pain and swelling can persist for up to a year.
If you want to learn more about arthritis, you can read about catching arthritis early or what it is like living with arthritis. If you are experiencing symptoms, we recommend you speak to a doctor.
Plantar Fasciitis
What is plantar fasciitis?
Inflammation of the strong band of tissue (fascia) that runs from the heel to the base of your toes. The fascia helps support the arch of the foot during weight bearing and the bowstring-like structure adds a spring to each step.
What causes plantar fasciitis?
If the fascia is stressed over time, small tears can develop in the tissue and cause pain under the foot. This may feel like a sharp pain either in the heel or the underside of the foot as soon as you place your foot on the ground. Prolonged walking or standing will generally make it worse.
What can help people suffering from plantar fasciitis?
Usually, the pain will ease over time (most cases improve within 3 to 6 months and 80 per cent of people’s symptoms completely resolve within a year), but there are self-help tips to speed up recovery including:
• Resting your foot: Avoid running or standing too much.
• Choosing cushioned footwear: Look for good arch support and avoid walking barefoot on hard surfaces.
• Small heel inserts: These raise the heel by 1cm
• Pain relief: Non-steroidal anti inflammatory drugs including paracetamol can reduce pain, as can applying an ice pack (e.g. frozen veg wrapped in a towel) for 15 to 20 minutes.
• Try stretching exercises: Loop a towel around your foot and pull your foot back towards you, keeping the knee straight. Hold it for 30 seconds and then repeat three times. Do this once a day.
• To prevent future attacks: Regularly stretch your calf muscles and plantar fascia, avoid exercising on hard surfaces, wear shoes with cushioned heels and good arch support and change them regularly.
If you have been diagnosed with plantar fasciitis, our physiotherapy experts have some advice on easing the pain.
Morton’s neuroma
What is Morton’s Neuroma?
This affects the nerves that run through the toes and is also known as Morton’s metatarsalgia. The nerve between the toes becomes swollen which can then become compressed by wearing shoes. Symptoms initially are tingling in the space between the toes, later this can lead to cramp in the toes and a sharp stabbing pain in the ball of your foot.
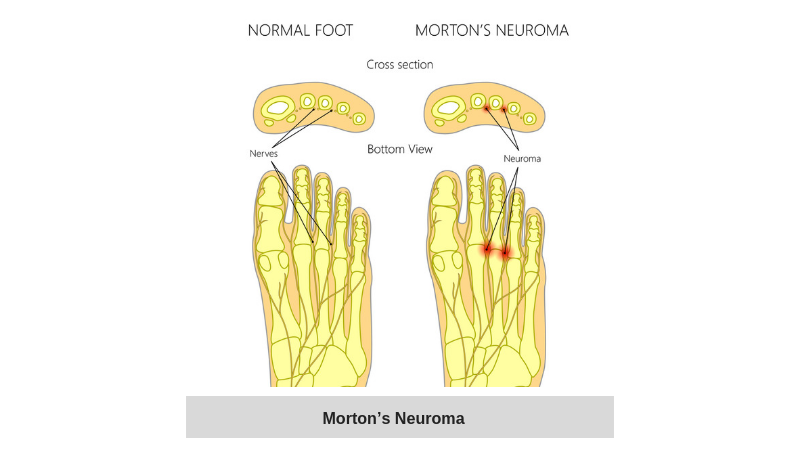
What causes Morton’s neuroma?
One study presented to the Royal College of Surgeons found the number of people suffering from Morton’s Neuroma has doubled since 2004, with experts pinpointing the increase on people wearing high heels. Moreover, women are 8 to 10 times more likely to suffer from Morton’s neuroma than men.1
What can help people suffering from Morton’s Neuroma?
• Change your shoes: Wearing broader fitting shoes may help reduce pressure on the neuroma. Orthotic inserts can also help.
• Steroid injections: These are effective in 70 per cent of cases.
• Surgery: If symptoms don’t respond to any of the above then surgery to remove tissue to either relieve pressure on the nerve or remove it may be suggested. The surgery can be done as a day case and takes 2 to 3 weeks to recover from.
Watch Andrew Skyrme’s video on Morton’s neuroma to help you understand more about this condition.
Flat feet (fallen arches) in adults
What is flat feet?
If you’re flat footed you have either low arches or none. Flat feet don’t usually cause pain, but may put a strain on your muscle or ligaments. Pain may be felt when you walk, in the inside of your ankle, the arch of your foot, outer side of your foot, calf, hip or knee.
What causes flat feet?
Some people are born with flat feet, but others develop it later in life as a result of injury, arthritis or conditions that affect the nervous system. It’s most common in women over the age of 40.
What can help people suffering from flat feet?
• Orthotic insoles: These stop your foot rolling inwards (called overpronation) when you walk but need to be custom made by a podiatrist.
• Calf stretching exercises: These can help prevent the Achilles tendon (a tight band of fibrous tissue that connects the calf muscle to the heel bone), becoming too tight which can also make your foot roll inwards.
• Surgery: This is only usually done if a joint problem or torn tendon is severely affecting your feet.
If you are experiencing unexplained pain or symptoms in your feet, ankles or toes, we would always recommend speaking to your doctor for advice.
At Horder Healthcare, we can provide you with fast access to the very best orthopaedic consultants for prompt treatment – with no waiting lists. Find out more about becoming a patient today.
What makes Horder Healthcare unique
Horder Healthcare is committed to providing the very best quality of care for our patients and customers. We are continuously working on improving and reducing risks and this is reflected in our consistently high CQC results, patient satisfaction questionnaires and minimal levels of infection.
We are a charity
We reinvest our profit to benefit more people and help us achieve our aim of advancing health.