By Consultant Orthopaedic Surgeon Mr Per Anderberg
You find it harder and more painful to walk than you used to and notice you are increasingly reaching for the painkillers. Sound familiar?
For many it will as these are typical symptoms of osteoarthritis, the most common form of arthritis that affects around one million people in this country alone. Although there is no cure, there is now much that can be done for many forms of this disease.
Once known as wear and tear arthritis, this occurs when the protective cartilage at the end of the bones become thinner while the bone itself becomes harder. This alters the shape of the joint and leads to stiffness and makes movement hard.
Many people don’t bother going to seek medical advice and shrug it off as ‘just a part of getting older.’ While it is true there is no cure per se there is much that can be done and the sooner you ask for help the better.
Osteoarthritis symptoms
“The usual symptoms are pain or swelling, locking or giving way of the joint, limping, or changes in the gait”, says Mr Per Anderberg, a consultant orthopaedic surgeon at The Horder Centre.
Sometimes the patient thinks there is nothing that can be done for them and so delay going to the doctor. Or they think that the only option is surgery and they don’t want that. The truth is that there are other options – such as painkillers, or steroid or hyaluronic acid injections.
“Simple lifestyle measures such as losing weight or becoming more active also can help. Even if surgery is suggested, the joint replacements we do now are very successful and can last for 20 years or more .”
Doing nothing is the worst possible option. It weakens muscles around already painful joints and leaves them less supported.
“Also if someone is limping or has an altered gait for a long time this can have a knock-on effect on other joints in the legs and back,” says Mr Anderberg.
Osteoarthritis symptoms
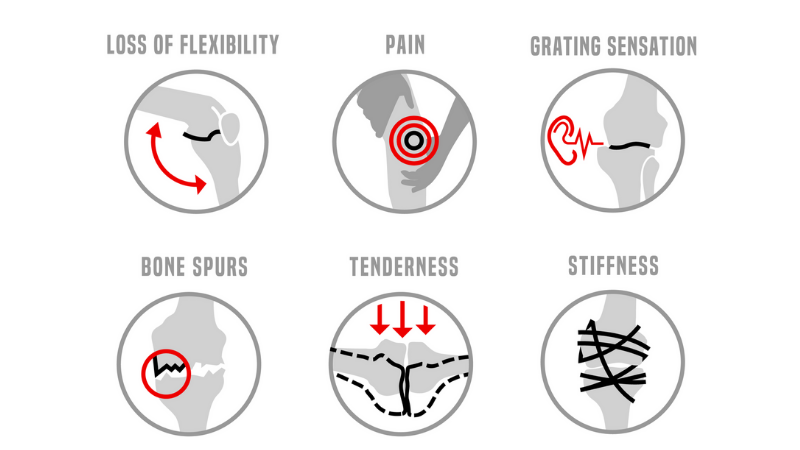
Osteoarthritis treatment
Non-surgical options
Keeping active is one of the best ways to reduce pain from arthritis.
It will strengthen the muscles, improve bone strength and the exercise will also help you to sleep – which can be hard if you have painful joints.
“There are other things that you can do to help, give up smoking, for example, this can help reduce pain, especially back pain,” says Mr Anderberg.
“Losing weight will help reduce the strain on the joints but the most important measure of all is exercise as increased muscle strength stabilises the joint but exercise and can also have a direct effect on the pain in the joint. Cycling exercises can have a big impact on reducing joint pain in the knee and hips. In general exercising before having a joint replacement can increase mobility and strength and mean a quicker recovery.”
Some people respond well to physiotherapy, doing specific exercises to strengthen certain muscles that support the arthritic joint – which helps improve movement. Anti-inflammatory medication or painkilling injections can also help in the early stages.
Some people don’t like taking medication: “but it is really better to do what it takes to keep yourself active, this is what will help keep the disease in check”, says Mr Anderberg.
When is the right time for surgery?
Once you have reached the point where everyday life and just getting from A to B is being affected a joint replacement may be suggested.
“It is hard to know when is the exact right time to operate,” says Mr Anderberg.
“Although I think in some cases it is becoming harder for patients to get a referral to an orthopaedic surgeon when they want to, as there is a culture that joint replacement should be delayed for as long as possible. Actually, this is not the right approach as sometimes the operation will be made harder if you put it off.”
This is because muscles may become weaker and the other joints will be put under pressure as you naturally avoid using a painful arthritic joint.
“As a surgeon, I would rather see people possibly before they need a replacement and make the decision that it is not the right time for surgery and discuss non-surgical measures with them,” says Mr Anderberg.
“If I see someone who is not too bad I will say ‘we don’t need to do anything now, go and see your GP again for another referral if it gets worse.’ I would rather that happen than see someone whose disease has progressed so much that the benefits of the surgery will be limited. Delaying surgery can mean a higher risk of complications and makes the operation technically more difficult.”
“In my experience, patients want to discuss both surgical and non-surgical measures. The decision about a joint replacement is usually a process and can require both time and repeat visits.”
In around 95 per cent of cases, a joint replacement is successful and reduces pain and improves mobility. However, there are risks such as infection and blot clots and if you have a replacement too young you may need another one in the future.
“Doing a replacement in someone under 60 is controversial because of this but, sometimes it is the right thing to do, it very much depends on the individual circumstances,” says Mr Anderberg.
Other forms of arthritis
Osteoarthritis is not the only form of the disease that needs early treatment.
Rheumatoid arthritis, an autoimmune condition in which the body attacks the lining of the joints causing irritation and inflammation, also need to be treated early. This condition was once a leading cause of disability but now thanks to a new generation of drugs the outlook for most RA patients has changed significantly.
However, treatment needs to start ideally within the first six weeks of the onset of symptoms such as swollen joints and stiffness in the morning. If it is left untreated the inflammation can cause permanent damage to the joints which in some cases it can become disabling.
“The improved pharmacological treatment for RA has led to less severely affected hips and knees and, as surgeons, we don’t see these patients early in life as we did before.”
What makes Horder Healthcare unique
Horder Healthcare is committed to providing the very best quality of care for our patients and customers. We are continuously working on improving and reducing risks and this is reflected in our consistently high CQC results, patient satisfaction questionnaires and minimal levels of infection.
We are a charity
We reinvest our profit to benefit more people and help us achieve our aim of advancing health.